What is Pulsed RFA?


Benefits
Minimally Invasive
Preserves Nerve Function
Long-Lasting Pain Relief
Low Risk of Tissue Damage
Reduced Recovery Time
Repeatable Treatment
Reduced Need for Opioids
Wide Range of Applications
Expanded Guide
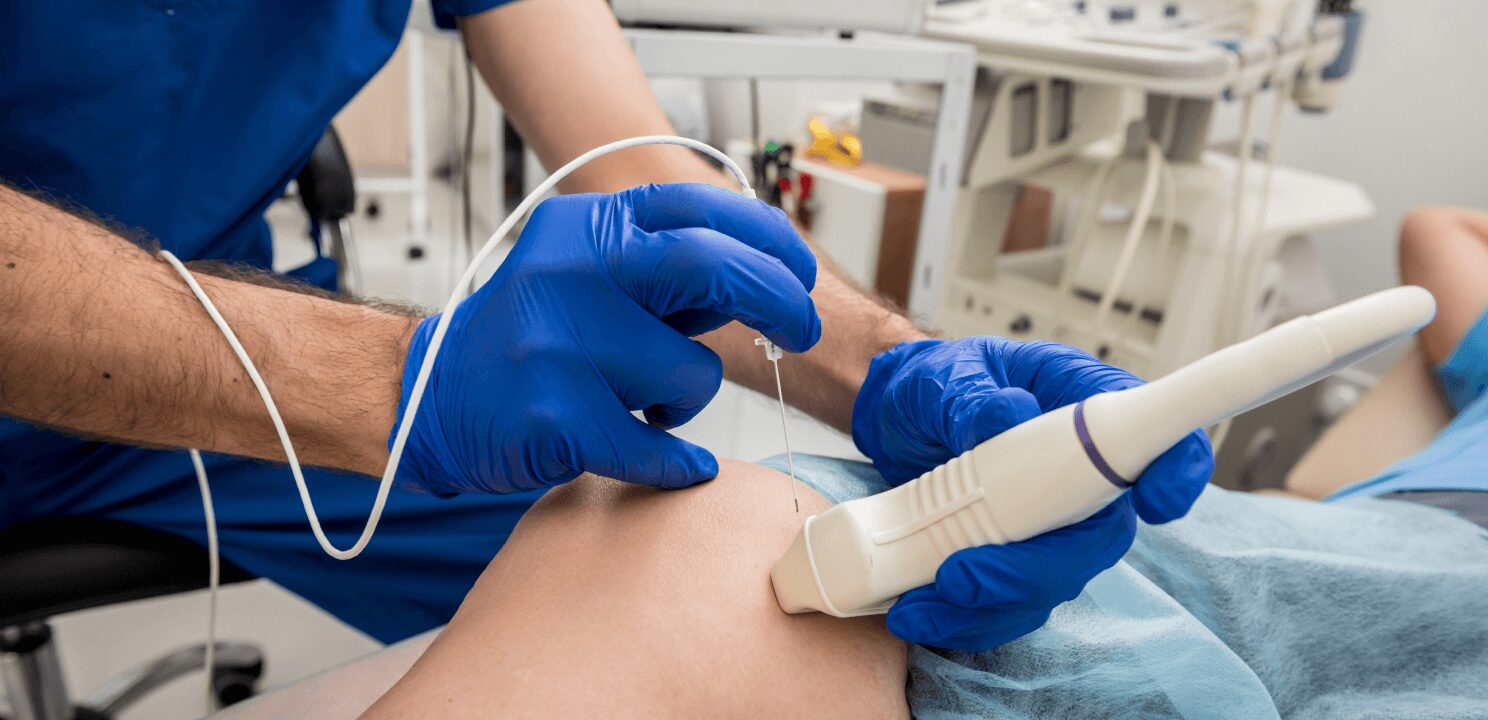
Pulsed Radiofrequency Neuromodulation (PRFN), also referred to as Pulsed Radiofrequency Ablation (PRFA), is a modern, minimally invasive procedure used to manage and alleviate chronic pain, especially in cases where conventional treatments have been insufficient. It is a non-destructive technique that uses electrical impulses to modify the way nerves transmit pain signals without causing permanent damage to the nerves or surrounding tissue, which differentiates it from continuous radiofrequency ablation that relies on heat to destroy nerve tissue.
How Does PRFN Work?
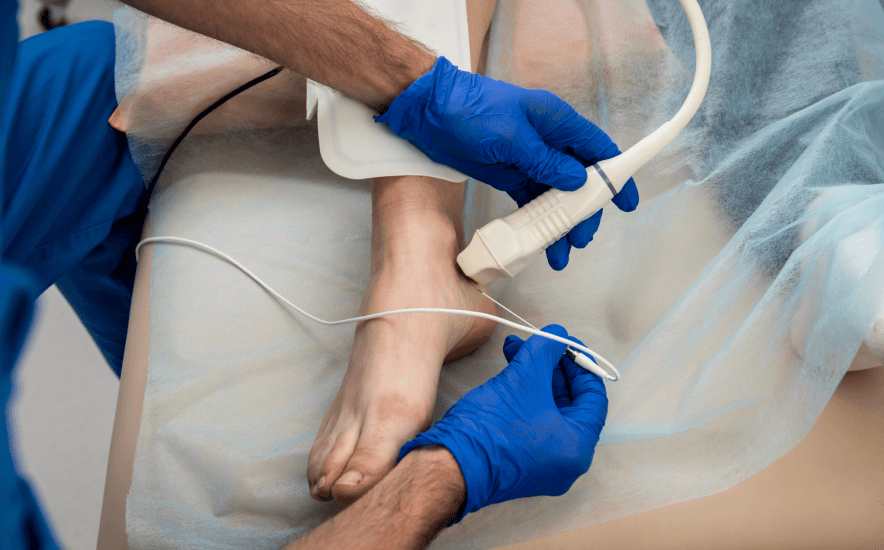
The core principle of PRFN is to target specific nerves responsible for transmitting pain signals to the brain. This is done by inserting a specialized needle or probe near the affected nerve under imaging guidance (such as fluoroscopy or ultrasound) to ensure accurate placement. Once in position, the device delivers pulsed electrical currents in short bursts. These pulses are delivered at a lower frequency than those used in continuous radiofrequency ablation, ensuring that the temperature does not rise high enough to damage the nerve. The goal is not to destroy the nerve but to “reset” or modulate its activity in a way that alters the perception of pain.
PRFN essentially reduces the nerve’s ability to send pain signals while maintaining its normal sensory and motor functions. This is particularly important in delicate areas such as the spine, where preserving nerve function is crucial for movement and sensation.
Conditions Treated by PRFN
PRFN is widely used to treat a variety of chronic pain conditions, particularly those involving neuropathic pain (pain resulting from nerve injury or dysfunction). Some of the most common conditions treated by this procedure include:
- Chronic back and neck pain: PRFN is often used in patients with pain caused by conditions such as herniated discs, degenerative disc disease, or spinal arthritis.
- Trigeminal neuralgia: This condition causes intense facial pain, and PRFN can provide relief by targeting the trigeminal nerve.
Sciatica and other nerve-related pain: By targeting the affected nerve roots, PRFN can reduce the pain that radiates from the lower back to the legs or arms. - Joint pain: PRFN is sometimes used to treat chronic pain in the knees, hips, and shoulders when other treatments have failed.
- Post-surgical pain: Patients who experience ongoing pain after surgery may benefit from PRFN, especially if the pain is neuropathic in origin.
The PRFN Procedure
The PRFN procedure is typically performed on an outpatient basis and generally takes about 30 to 60 minutes. Patients lie comfortably while the physician uses imaging guidance to locate the exact nerve responsible for the pain. A local anesthetic is applied to numb the skin before the specialized needle is inserted. Once the needle is in place, electrical pulses are delivered in controlled bursts. Patients usually remain awake during the procedure to provide feedback, helping the physician fine-tune the treatment.
Unlike continuous radiofrequency ablation, which can cause significant post-procedural discomfort due to nerve destruction, PRFN is generally well-tolerated, with most patients experiencing only mild soreness at the treatment site. Since the procedure does not rely on heat, it has a lower risk of complications, such as tissue damage or excessive scarring.
Benefits
Pulsed Radiofrequency Neuromodulation (PRFN) offers several significant benefits for managing chronic pain. As a minimally invasive procedure, it requires only a small needle insertion, which reduces the risks associated with more invasive treatments like surgery. One of the standout advantages is that PRFN preserves normal nerve function, modulating pain signals without permanently damaging the nerve. This is in contrast to continuous radiofrequency ablation, which destroys nerve tissue. Patients often experience long-lasting pain relief, with studies showing that 60-70% of individuals benefit from relief that can last several months to over a year.
Additionally, PRFN operates at lower temperatures, minimizing the risk of heat-related tissue damage. The recovery time is shorter compared to surgical alternatives, allowing patients to return to their regular activities more quickly. Another key benefit is that the procedure can be repeated if pain returns, providing a sustainable solution for long-term pain management. Importantly, PRFN also helps reduce the need for opioids or other pain medications, lowering the risks of side effects and dependence associated with long-term medication use. Furthermore, PRFN is versatile, treating a wide range of chronic pain conditions such as back and neck pain, joint pain, trigeminal neuralgia, and sciatica, making it an effective option for many patients.
Conclusion
Pulsed Radiofrequency Neuromodulation is an innovative and minimally invasive treatment option for managing chronic pain, especially in patients who have not found relief through other methods. By modulating nerve activity without causing significant damage, PRFN provides a safe and effective alternative to traditional ablation techniques. With its high success rate, minimal side effects, and the ability to preserve normal nerve function, PRFN offers hope to patients suffering from debilitating chronic pain, improving their quality of life and reducing dependence on long-term medication use.
Frequently Asked Questions
Have more questions? Schedule a consultation with Dr. Patel to gain additional insights and discuss treatment options. We are committed to advancing your health through patient education and a safe, minimally invasive approach.
Gramercy Center
Take the first step towards a healthier life by scheduling your initial consultation with Dr. Patel. At our clinic, we specialize in minimally invasive procedures that offer faster recovery, improved function, and decreased pain. Our client-centered approach ensures that you receive the highest quality care tailored to your unique needs. We look forward to offering you an exceptional experience.