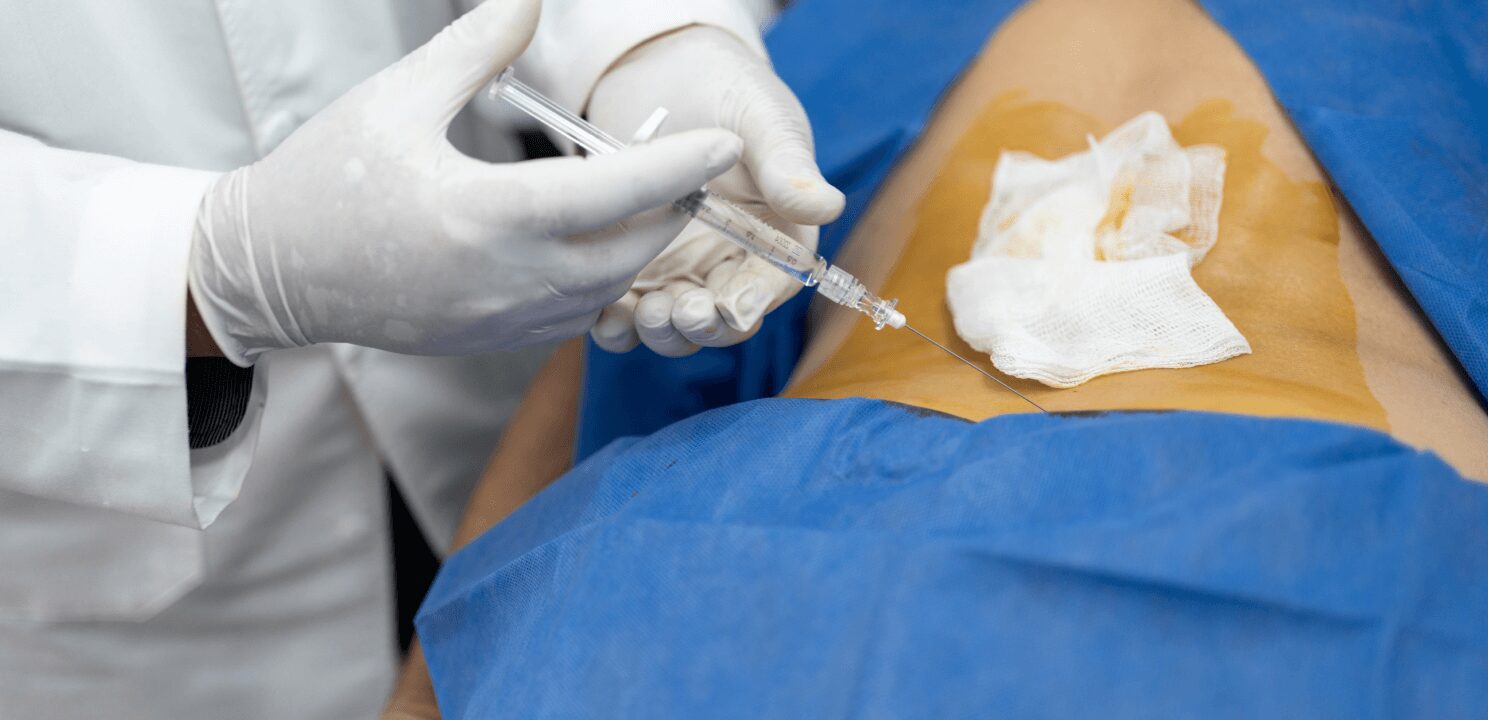
What are Intradiscal Injections?

Benefits
Targeted Pain Relief
Reduces Inflammation
Minimally Invasive
Quick Recovery
Improves Mobility
Supports Other Treatments
Delays or Avoids Surgery
Low Risk of Complications
Expanded Guide
Intradiscal injections are a minimally invasive procedure used to manage chronic back pain that originates in the intervertebral discs, often due to degenerative disc disease, herniated discs, or other inflammatory disc conditions. The procedure involves injecting a therapeutic substance directly into the affected disc to target pain and inflammation, aiming to reduce discomfort and improve function. For patients who have not found sufficient relief from conservative treatments such as physical therapy, oral medications, or lifestyle changes, intradiscal injections offer an alternative option that may help delay or even avoid surgical intervention.
How Intradiscal Injections Work
Intervertebral discs are located between each vertebra in the spine and act as cushions, absorbing shock and allowing for flexibility and movement. Over time, these discs can degenerate, lose hydration, and become inflamed or damaged, which may lead to pain that radiates through the back, sometimes into the legs or arms. Intradiscal injections aim to reduce this pain by directly addressing the affected disc.
The type of substance injected varies based on the patient’s condition and the healthcare provider’s approach. Common substances include corticosteroids, which help to reduce inflammation, or platelet-rich plasma (PRP), which may promote healing and tissue regeneration. In some cases, biologics or ozone injections are used for their potential regenerative effects. By reducing inflammation and targeting the damaged tissue, these injections can alleviate pain and may even improve disc health over time.
Conditions Treated with Intradiscal Injections
Intradiscal injections are typically recommended for patients experiencing:
- Degenerative Disc Disease (DDD): A condition where the discs wear down over time, leading to chronic pain and stiffness.
- Discogenic Pain: Pain that originates specifically from the disc itself, often due to small tears or inflammation within the disc structure.
- Herniated or Bulging Discs: When a disc’s outer layer tears or bulges, it can press on nearby nerves, leading to pain and discomfort.
- Internal Disc Disruption: Small tears or fissures within the disc can lead to pain by causing nerve irritation within the disc itself.
The Procedure
Intradiscal injections are performed on an outpatient basis, meaning patients can go home shortly after the procedure. The patient lies on a procedure table, and the injection site is cleaned and numbed with a local anesthetic. Using fluoroscopic (X-ray) guidance, the physician carefully inserts a thin needle into the center of the affected disc. Contrast dye may be injected first to confirm correct needle placement, followed by the therapeutic substance, such as a corticosteroid or PRP. The entire procedure usually takes about 30 to 60 minutes.
Patients may experience mild pressure or discomfort during the injection, but most tolerate it well. Afterward, patients are typically monitored briefly to ensure there are no immediate side effects and then discharged with post-procedure care instructions. Many patients are advised to rest and avoid strenuous activities for a few days to support recovery and optimize the injection’s effectiveness.
Benefits
Intradiscal injections offer several significant benefits for patients with chronic disc-related pain. One of the main advantages is targeted pain relief, as the injection delivers medication directly into the affected disc, addressing the pain source. The corticosteroid or regenerative substance injected helps reduce inflammation, relieving pain and pressure in the area. This procedure is minimally invasive, performed with a small needle and imaging guidance, making it a low-risk option compared to surgery. Recovery is typically quick, with most patients experiencing minimal downtime and returning to daily activities within a few days. By reducing pain, intradiscal injections often enhance mobility, allowing patients to move more comfortably and engage in daily activities with greater ease. Pain relief from the injections also supports other treatments, such as physical therapy, by making it easier for patients to participate in exercises that strengthen the spine. For many, intradiscal injections provide enough relief to delay or even avoid spinal surgery altogether. Additionally, with a low risk of serious complications, these injections are a safe and effective option for managing chronic disc-related pain.
Conclusion
Intradiscal injections are a promising treatment option for patients struggling with chronic disc-related pain. They offer a targeted, minimally invasive approach to pain relief by delivering medication or regenerative substances directly into the problematic disc. While results can vary, many patients find these injections effective in reducing pain, improving mobility, and enhancing quality of life. With a quick recovery period and relatively low risk of complications, intradiscal injections are an attractive option for those seeking alternatives to surgery or long-term medication use. For the best outcomes, intradiscal injections are often combined with physical therapy and other lifestyle modifications to support spine health and prolong the benefits of the treatment.
Frequently Asked Questions
Have more questions? Schedule a consultation with Dr. Patel to gain additional insights and discuss treatment options. We are committed to advancing your health through patient education and a safe, minimally invasive approach.
Gramercy Center
Take the first step towards a healthier life by scheduling your initial consultation with Dr. Patel. At our clinic, we specialize in minimally invasive procedures that offer faster recovery, improved function, and decreased pain. Our client-centered approach ensures that you receive the highest quality care tailored to your unique needs. We look forward to offering you an exceptional experience.