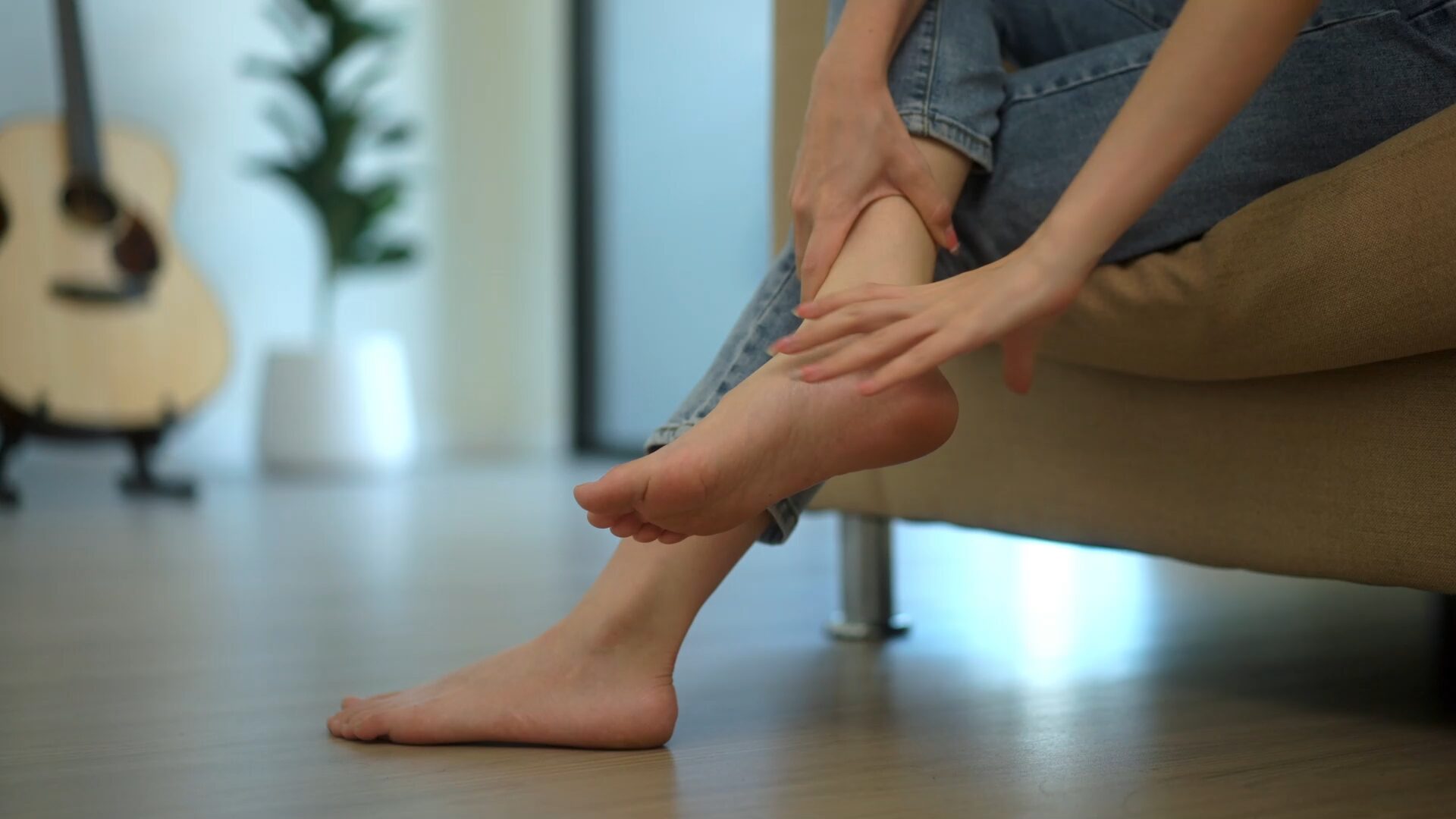
What is Painful Diabetic Neuropathy?
Painful diabetic neuropathy (PDN) is a type of nerve damage caused by chronically high blood sugar levels in individuals with diabetes. It primarily affects the peripheral nerves, leading to symptoms such as burning, stabbing, shooting, or tingling pain, often in the feet and legs, although it can also impact the hands and other areas.
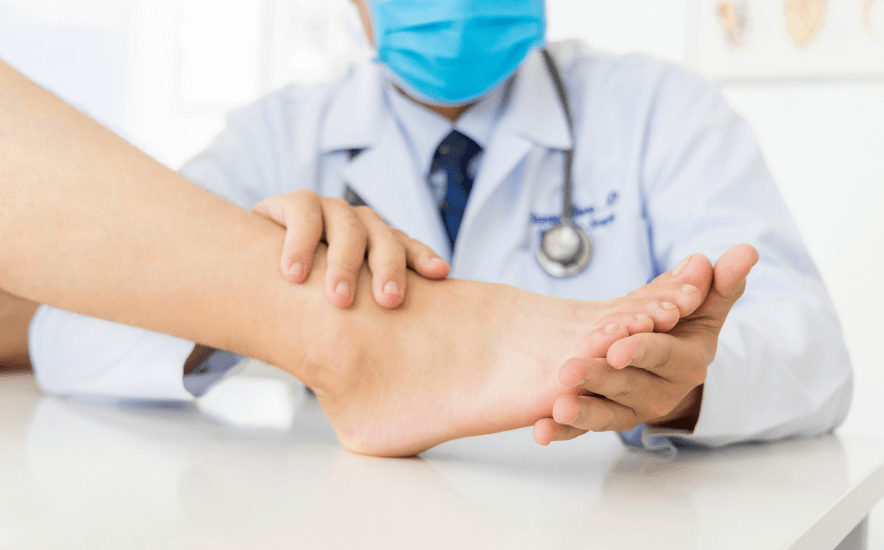


Relevant Symptomatology

Burning & Tingling Sensations

Shooting or Stabbing Pain

Electric Shock-Like Pain

Sensitivity to Touch

Burning Pain

Numbness & Reduced Sensation

Muscle Weakness
Expanded Guide
- Burning & Tingling Sensations: One of the most common and distressing symptoms of PDN is a persistent burning sensation, which can feel like the affected areas are on fire. Tingling, often described as “pins and needles,” is another common symptom. This tingling can range from mild to severe and is typically more pronounced in the feet, legs, and hands. These sensations are caused by nerve damage and are often continuous, making it difficult for individuals to find relief, even when resting.
- Shooting or Stabbing Pain: Many people with PDN experience sudden, sharp, or stabbing pain that can be unpredictable. This pain may occur spontaneously or be triggered by certain movements or stimuli. It is often described as feeling like sharp jabs or stabs, which can be intense and debilitating. This type of pain can appear in episodes and may be worse at night, further disrupting rest and quality of life.
- Electric Shock-Like Pain: Some patients with PDN describe their pain as resembling electric shocks. This type of pain can feel like sudden jolts or surges of electricity shooting through the affected nerves. It often strikes unexpectedly and can be triggered by movements or changes in temperature, making it challenging to anticipate or avoid.
- Sensitivity to Touch: People with PDN often develop a heightened sensitivity to touch, where even light pressure or gentle contact that normally wouldn’t be painful—like wearing socks, shoes, or having bed sheets touch the skin—becomes excruciating. This extreme sensitivity, called allodynia, results from damaged nerves misinterpreting normal sensations as pain. In severe cases, even the lightest touch or breeze can cause discomfort.
- Burning Pain: This type of pain is a hallmark symptom of PDN. It typically begins in the feet and lower legs and gradually worsens, especially at night. The burning can become intense, interfering with sleep and overall comfort. The constant sensation of burning may extend upwards from the feet to the calves, causing significant discomfort and contributing to sleep disturbances.
- Numbness & Reduced Sensation: In addition to pain, some individuals experience numbness or a loss of sensation in the affected areas. The numbness often occurs alongside painful symptoms, creating a paradoxical experience of feeling both pain and reduced sensitivity. This lack of sensation can be dangerous, as it increases the risk of injuries or infections that go unnoticed due to the reduced ability to feel cuts, wounds, or blisters.
- Muscle Weakness: As the condition progresses, damaged nerves may impair the function of the muscles they control, leading to weakness. This can result in difficulty with balance, coordination, or walking. Over time, muscle weakness can contribute to gait instability and increase the risk of falls. Individuals may also find it harder to perform tasks that require fine motor control, especially if the hands are affected.
Frequently Asked Questions
Have more questions? Schedule a consultation with Dr. Patel to gain additional insights and discuss treatment options. We are committed to advancing your health through patient education and a safe, minimally invasive approach.
The diagnosis of painful diabetic neuropathy (PDN) involves a combination of clinical evaluation, physical exams, and diagnostic tests. First, a doctor reviews the patient’s diabetes history and symptoms, focusing on pain type (burning, tingling, shooting, etc.) and affected areas. A physical exam includes tests for touch, vibration, temperature, and reflexes, often using tools like monofilaments and tuning forks. Nerve conduction studies and electromyography may be used to assess nerve function. Blood tests check HbA1c, vitamin B12, and thyroid levels to rule out other causes of neuropathy. In rare cases, nerve or skin biopsies are conducted. Pain scales help quantify severity, ensuring accurate diagnosis and effective treatment planning.
Treatment for painful diabetic neuropathy (PDN) focuses on pain relief, slowing disease progression, and improving quality of life. Key approaches include tight blood sugar control to prevent further nerve damage, and medications like anticonvulsants (gabapentin, pregabalin) or antidepressants (amitriptyline, duloxetine) to manage pain. Topical treatments such as lidocaine patches and capsaicin cream, as well as physical therapy, can also provide relief. Non-drug options like spinal cord stimulation, and lifestyle changes (healthy diet, exercise, smoking cessation) can help improve symptoms. In some cases, supplements like alpha-lipoic acid or vitamin B12, and stress reduction techniques, may offer additional benefits. Treatment plans are typically individualized and may combine several methods to effectively manage symptoms.
Painful diabetic neuropathy (PDN) is often a chronic condition that can persist for months, years, or even a lifetime, depending on the individual and the effectiveness of treatment. Once nerve damage has occurred due to diabetes, it is generally irreversible, and symptoms like pain may continue long-term. However, with proper management, including tight blood sugar control and treatment for pain, the severity of symptoms can be reduced, and some patients may experience relief over time. In some cases, symptoms may fluctuate, with periods of more intense pain followed by periods of relative relief. The key to managing PDN is early intervention and ongoing care to minimize pain and prevent further nerve damage.
Painful diabetic neuropathy (PDN) can lead to serious complications if not managed properly. Numbness & reduced sensation increase the risk of foot injuries, ulcers, and infections, which can lead to amputation in severe cases. Chronic pain from PDN can impair daily activities and cause mental health issues like depression. Additionally, nerve damage may cause balance and mobility issues, raising the risk of falls. Sleep disturbances are common due to worsening pain at night, and in some cases, the condition can lead to autonomic neuropathy, affecting heart rate, digestion, and bladder control. Effective management is essential to prevent these complications.
Gramercy Center
Take the first step towards a healthier life by scheduling your initial consultation with Dr. Patel. At our clinic, we specialize in minimally invasive procedures that offer faster recovery, improved function, and decreased pain. Our client-centered approach ensures that you receive the highest quality care tailored to your unique needs. We look forward to offering you an exceptional experience.
