
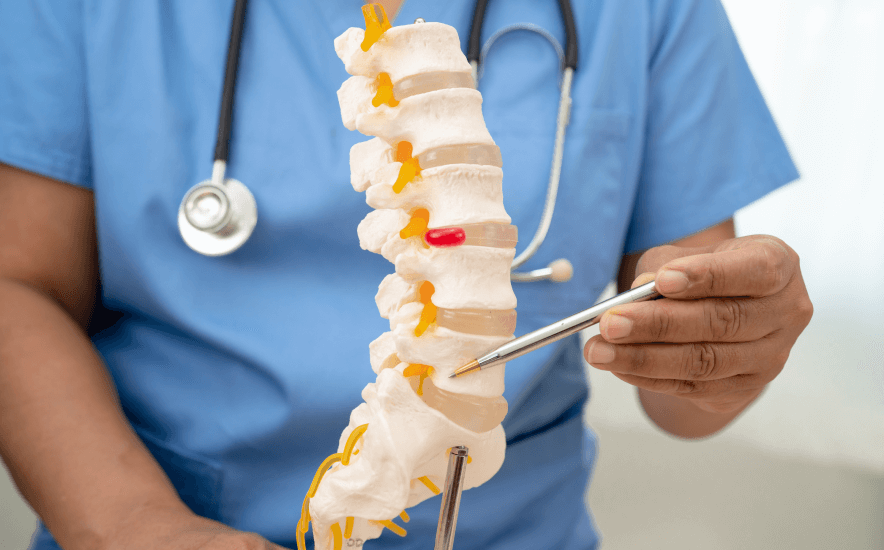
What is Dorsalgia?
Dorsalgia is a medical term that refers to pain originating in the back. The term encompasses a broad range of back pain conditions, which may affect different regions of the spine, including the cervical (neck), thoracic (mid-back), and lumbar (lower back) areas. Dorsalgia can result from various causes, such as muscle strain, poor posture, degenerative changes in the spine (like herniated discs or osteoarthritis), or underlying conditions like scoliosis or spinal infections. It is often categorized by the location and type of pain, such as upper dorsalgia or lumbago (lower back pain).


Related Diagnoses

Lumbar Facet Arthritis

Lumbar Radiculopathy & Sciatica

Lumbar Muscle Spasms

Lumbar Spinal Stenosis

Degenerative Disc Disease

Vertebral Fractures
Post-Surgical Spinal Pain

Multifidus Muscle Dysfunction

Vertebrogenic Pain Syndrome

Cluneal Neuralgia

Lumbar Disc Herniation

Whiplash & Lumbar Strain
Expanded Guide
- Lumbar Facet Arthritis: Lumbar Facet Arthritis, also known as Lumbar Spondylosis, is a degenerative condition that affects the facet joints in the lower back (lumbar spine). These facet joints connect the vertebrae in the spine and allow for movement and flexibility, such as bending and twisting. Over time, due to age, wear and tear, or injury, the cartilage in these joints can break down, leading to inflammation, stiffness, and pain—characteristics of arthritis. This condition typically develops as part of the natural aging process, where the discs between the vertebrae lose hydration and shrink, increasing stress on the facet joints. As the cartilage wears away, bones can rub against each other, causing discomfort and further degeneration. In some cases, this can also lead to bone spurs (osteophytes), which may irritate surrounding nerves and contribute to conditions like spinal stenosis. Symptoms of lumbar facet arthritis include lower back pain, especially after periods of inactivity or in the morning, stiffness, limited range of motion, and pain that may radiate to the buttocks or thighs.
- Lumbar Radiculopathy & Sciatica: Lumbar Radiculopathy and Sciatica are related conditions that involve nerve compression in the lower back, but they differ in specific causes and manifestations. Lumbar Radiculopathy refers to nerve irritation or compression in the lower (lumbar) spine, causing pain, numbness, tingling, or weakness that radiates along the path of the affected nerve. This condition occurs when the spinal nerves that exit the lumbar vertebrae are pinched, often due to causes like herniated discs, spinal stenosis, bone spurs, or degenerative disc disease. The symptoms of lumbar radiculopathy vary depending on which nerve root is compressed, and the pain can travel from the lower back down into the legs or feet. Sciatica is a specific type of lumbar radiculopathy that refers to the irritation or compression of the sciatic nerve, the longest nerve in the body. The sciatic nerve originates from the lower spine (L4-S3) and runs through the buttocks and down the back of each leg. When this nerve is compressed—often due to a herniated disc, spinal stenosis, or spondylolisthesis—it results in sharp, shooting pain that radiates from the lower back, through the buttocks, and down the leg, often reaching the foot. Sciatica is usually felt on only one side of the body and can be accompanied by numbness, tingling, or muscle weakness in the affected leg.
- Lumbar Muscle Spasms: A lumbar muscle spasm is an involuntary contraction or tightening of the muscles in the lower back, often causing intense pain and making movement difficult. These spasms can result from various causes, such as muscle strain due to heavy lifting, overuse from repetitive activities, poor posture, or injuries like falls or accidents. Additionally, lumbar muscle spasms may occur as a symptom of underlying conditions such as herniated discs, spinal stenosis, or arthritis. The primary symptom is a sudden, sharp pain in the lower back, accompanied by muscle stiffness, tightness, and restricted movement. In some cases, the pain may radiate to the buttocks or legs, and the affected area may be tender to the touch.
- Lumbar Spinal Stenosis: Lumbar spinal stenosis is a condition in which the spinal canal in the lower back becomes narrowed, leading to pressure on the spinal cord and nerves. This narrowing can result from various causes, most commonly age-related degenerative changes such as osteoarthritis, herniated discs, bone spurs, and thickened ligaments. As the spine ages, the discs lose water and shrink, reducing the space within the spinal canal. Bone overgrowth from osteoarthritis or a slipped vertebra (spondylolisthesis) can further contribute to this narrowing. Symptoms of lumbar spinal stenosis often develop gradually and are exacerbated by activities like standing or walking. They commonly include lower back pain, tingling, numbness, or weakness that radiates into the buttocks, thighs, or legs, a condition known as neurogenic claudication. Cramping in the legs and difficulty walking may also occur, and in severe cases, there can be a loss of bladder or bowel control, known as cauda equina syndrome, which is a medical emergency.
- Degenerative Disc Disease: Lumbar Degenerative Disc Disease (DDD) occurs when the intervertebral discs in the lower back begin to break down due to natural age-related wear and tear. Although it is called a “disease,” it is actually a degenerative process that happens over time. These discs act as cushions between the vertebrae, providing shock absorption and flexibility. As people age, the discs lose hydration and elasticity, becoming thinner and less able to support the spine. This degeneration can also be accelerated by repetitive stress, heavy lifting, or injury, leading to pain and other symptoms. The primary symptom of lumbar DDD is lower back pain, which can range from mild to severe, often worsening with activities like sitting, bending, or lifting. In some cases, the pain may radiate to the hips, buttocks, or legs, and people may experience numbness, tingling, or weakness if the damaged discs compress nearby nerves.
- Vertebral Fractures: A thoracolumbar compression fracture is a type of spinal fracture that occurs in the mid-back (thoracic) or lower back (lumbar) regions, often involving the collapse or compression of a vertebra. This can lead to pain, reduced mobility, and potentially serious complications if left untreated. These fractures commonly result from trauma, such as falls or car accidents, or from weakened bones due to conditions like osteoporosis, which makes vertebrae more susceptible to fractures even with minor stress. Symptoms typically include sudden, sharp pain in the middle or lower back that worsens with movement, limited spinal mobility, and in some cases, loss of height or a hunched posture (kyphosis). In severe cases, nerve compression may cause radiating pain, numbness, or weakness in the legs.
- Post-Surgical Spinal Pain: Post-surgical spinal pain, also known as failed back surgery syndrome (FBSS) or post-laminectomy syndrome, refers to persistent or recurring pain following spinal surgery. Although spinal surgery is often performed to alleviate pain from conditions such as herniated discs, spinal stenosis, or degenerative disc disease, some patients continue to experience pain or develop new discomfort after the procedure, even if the surgery technically succeeded in addressing the initial issue. This pain may result from various factors, including incomplete resolution of the original problem, scar tissue formation around nerves, nerve damage, spinal instability, adjacent segment disease (degeneration of the spinal segments near the surgery site), or complications like infection. The primary symptom is ongoing or new pain in the area of the surgery, which may radiate to the legs or arms, accompanied by numbness, tingling, or weakness that can impact mobility and quality of life.
- Multifidus Muscle Dysfunction: Multifidus muscle dysfunction refers to the impaired function of the multifidus muscles, which are deep muscles along the spine responsible for stabilizing and supporting the spine during movement. When these muscles become weakened or inactive, it can lead to reduced spinal stability, chronic back pain, and an increased risk of injury. This dysfunction can be caused by factors such as injury, poor posture, prolonged inactivity, spinal conditions like herniated discs or degenerative disc disease, nerve compression, or post-surgical changes, particularly after spinal surgery. Symptoms of multifidus muscle dysfunction typically include chronic lower back pain, a sense of weakness or instability in the spine, poor posture, and a limited range of motion.
- Vertebrogenic Pain Syndrome: Vertebrogenic pain syndrome refers to pain that originates from the vertebrae, the bones of the spine, often caused by structural issues such as degenerative disc disease, vertebral fractures, or osteoarthritis. This condition typically results in chronic back pain, which may worsen with movement or prolonged sitting or standing. It can also radiate to other areas, like the shoulders, arms, or legs, if nerve compression occurs. Common causes of vertebrogenic pain include degenerative disc disease, where the discs between vertebrae wear down, vertebral fractures from trauma or osteoporosis, spinal arthritis, or conditions like spondylolisthesis, where one vertebra slips over another, leading to instability. Symptoms often include stiffness, reduced spinal mobility, and muscle spasms.
- Cluneal Neuralgia: Cluneal neuralgia is a condition characterized by pain caused by irritation or compression of the cluneal nerves, which supply sensation to the lower back, upper buttocks, and hips. The pain can range from mild to severe, with sensations often described as sharp, burning, or stabbing. It can be triggered by trauma, injury, muscle strain, or surgical complications that damage or compress these nerves, particularly the superior cluneal nerves. Cluneal neuralgia is sometimes misdiagnosed as other conditions like sciatica due to its similar symptoms.
- Lumbar Disc Herniation: Lumbar disc herniation occurs when an intervertebral disc in the lower back ruptures or bulges out of its normal position, pressing on nearby spinal nerves. These discs act as cushions between the vertebrae, but when the outer layer weakens or tears, the inner gel-like material can push out, causing a herniation. Common causes include age-related degeneration, injury, repetitive strain, or even genetic predisposition. Symptoms can range from lower back pain to sciatica, with pain radiating down the legs, numbness, tingling, or muscle weakness in the lower extremities.
- Whiplash & Lumbar Strain: Whiplash and lumbar strain are both injuries that affect different parts of the spine and are typically caused by sudden, forceful movements. Whiplash is a neck injury that occurs when the head is rapidly jerked forward and backward, commonly seen in rear-end car accidents or sports injuries. This causes strain or injury to the muscles, ligaments, and tendons in the neck, leading to symptoms such as neck pain, stiffness, headaches, and reduced mobility. Lumbar strain, on the other hand, refers to the overstretching or injury of the muscles and ligaments in the lower back. It is often caused by heavy lifting, sudden movements, or improper body mechanics during physical activity. Symptoms of lumbar strain include lower back pain, stiffness, and difficulty moving, especially when bending or twisting.
Frequently Asked Questions
Have more questions? Schedule a consultation with Dr. Patel to gain additional insights and discuss treatment options. We are committed to advancing your health through patient education and a safe, minimally invasive approach.
Diagnosis typically involves a physical examination, review of medical history, and imaging tests such as X-rays, MRI, or CT scans to determine the cause of the pain. Blood tests may also be performed to rule out infections or other underlying conditions.
Treatment depends on the underlying cause but may include rest, physical therapy, stretching exercises, medications (like anti-inflammatory drugs or muscle relaxants), heat or ice therapy, and lifestyle changes. In more severe cases, interventions like corticosteroid injections or surgery may be necessary.
The duration of dorsalgia, or back pain, can vary significantly depending on its cause, severity, and whether appropriate treatment is applied. Acute dorsalgia typically lasts from a few days to six weeks and is often caused by muscle strain, poor posture, or minor injuries. With rest and proper care, it usually resolves within this time frame. Subacute dorsalgia lasts between six weeks and three months and may result from more significant injuries or conditions, such as ligament damage or mild disc issues, requiring more targeted treatment like physical therapy or medications. Chronic dorsalgia, which persists for longer than three months, is often linked to underlying conditions like degenerative disc disease, arthritis, or spinal disorders.
Untreated dorsalgia (back pain) can lead to chronic pain, reduced mobility, muscle weakness, and stiffness, making daily tasks harder. Conditions like herniated discs or spinal stenosis may cause nerve compression, resulting in numbness, tingling, or permanent damage if unresolved. Chronic pain can also lead to spinal deformities, such as kyphosis, and mental health issues like anxiety, depression, or insomnia. Dependence on pain medications and reduced productivity are additional risks. In some cases, dorsalgia may indicate serious conditions like infections, fractures, or tumors. Prompt diagnosis and treatment are essential to prevent complications and improve quality of life.
Gramercy Center
Take the first step towards a healthier life by scheduling your initial consultation with Dr. Patel. At our clinic, we specialize in minimally invasive procedures that offer faster recovery, improved function, and decreased pain. Our client-centered approach ensures that you receive the highest quality care tailored to your unique needs. We look forward to offering you an exceptional experience.
