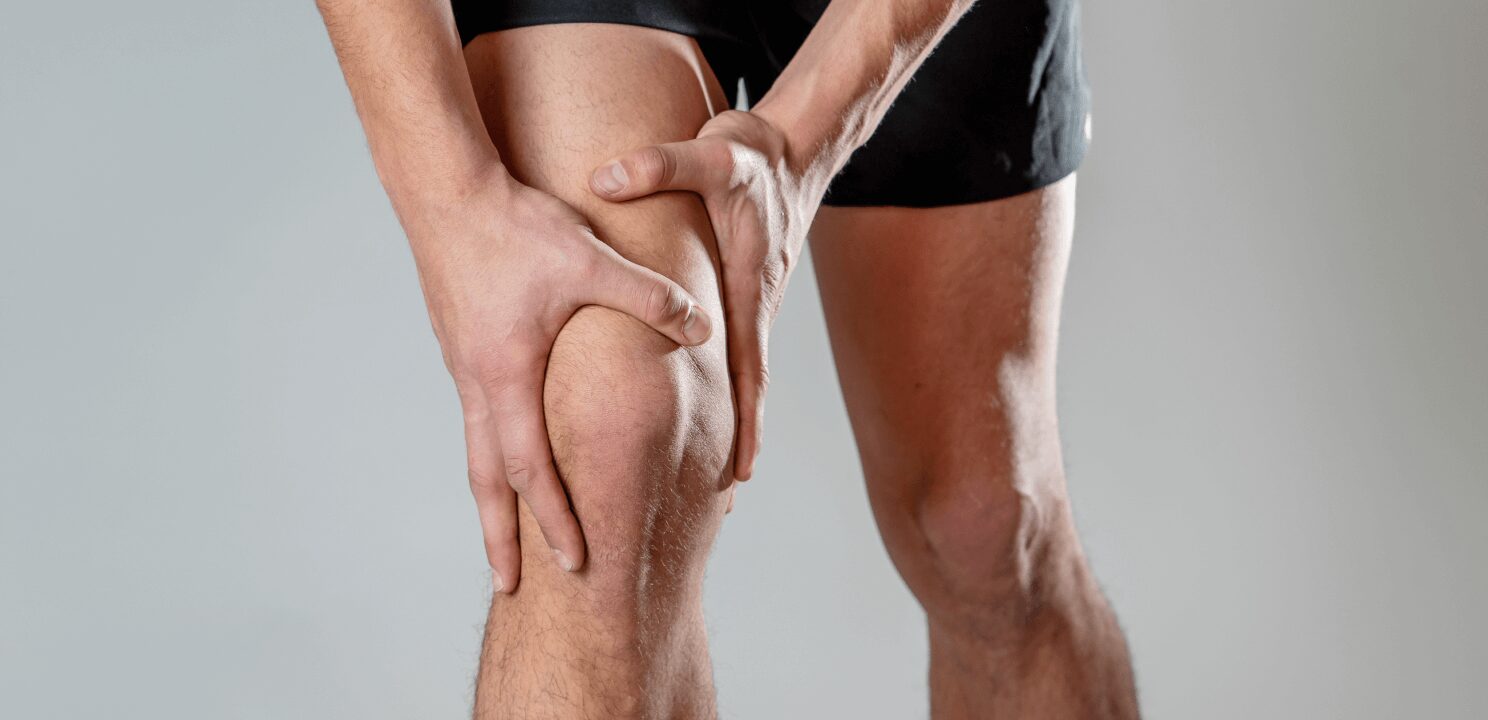
What is Knee Pain?
Knee pain is a common symptom that can result from a variety of causes, affecting the bones, cartilage, ligaments, muscles, or tendons around the knee joint. It can range from mild discomfort to severe, debilitating pain and may be localized to one specific area of the knee or be more diffuse, impacting mobility and overall quality of life.
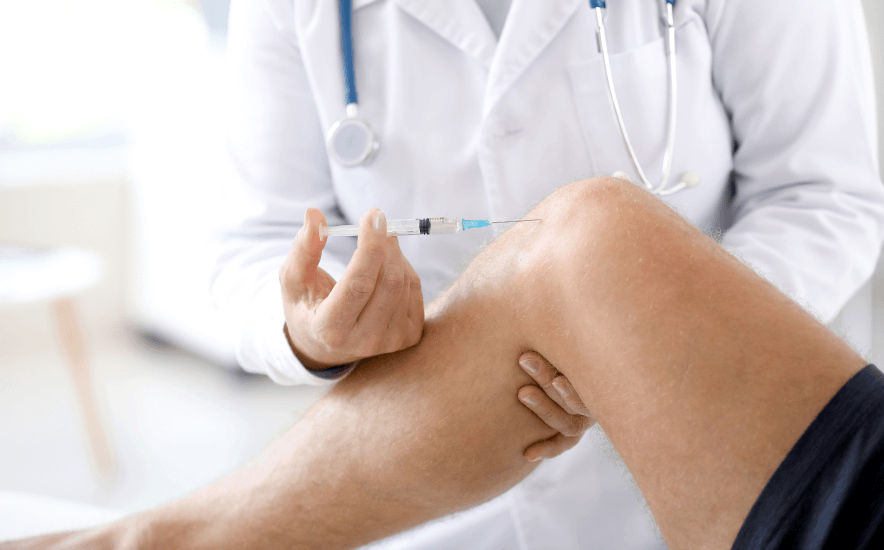

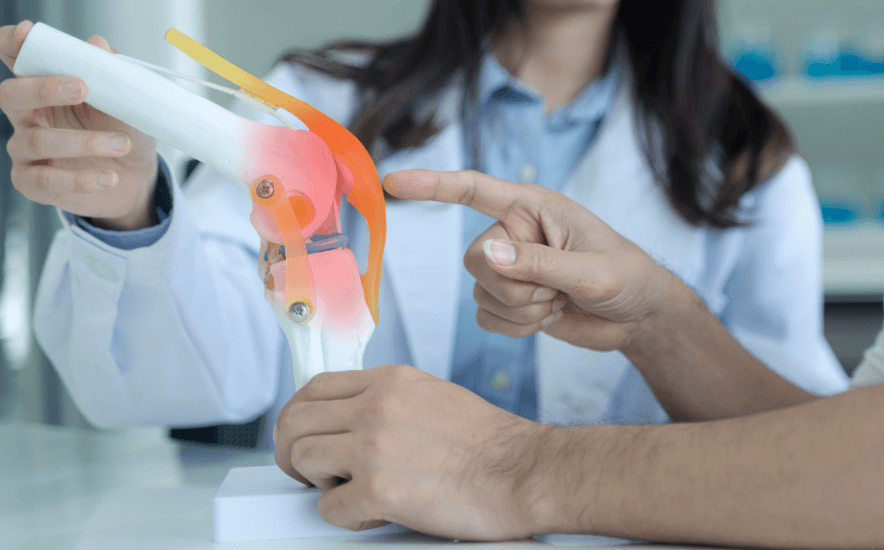
Related Diagnoses

Osteoarthritis
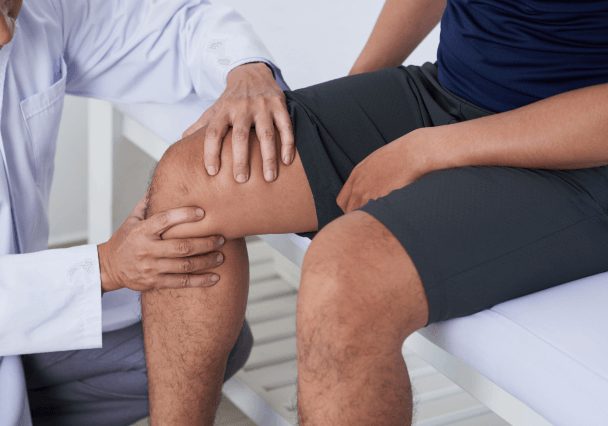
Post-Surgical Pain

Sprained & Torn Ligaments
Patellar Tendonitis

Patellofemoral Pain Syndrome

Meniscus Tear

Iliotibial Band Syndrome

Chondromalacia
Expanded Guide
- Osteoarthritis: Knee osteoarthritis (OA) pain is a specific type of knee pain caused by the gradual breakdown of cartilage in the knee joint. Cartilage is the smooth, cushion-like tissue that covers the ends of bones, allowing them to move smoothly against each other. In osteoarthritis, this cartilage wears down over time, leading to increased friction between the bones, inflammation, and pain. The pain associated with knee osteoarthritis can vary from mild to severe and typically worsens with activity, such as walking or climbing stairs, and improves with rest. People with knee OA often experience stiffness, especially after periods of inactivity or in the morning. Other symptoms may include swelling, tenderness, and a feeling of weakness or instability in the knee. As osteoarthritis progresses, the pain can become constant and more debilitating, limiting mobility and affecting the quality of life.
- Post-Surgical Pain: Post-surgical knee pain is a common issue following knee surgeries, such as total knee arthroplasty (TKA) and knee arthroscopy. Each procedure has different recovery processes and associated pain levels. In the case of total knee arthroplasty, which involves replacing damaged knee surfaces with artificial implants, post-surgical pain tends to be significant in the early stages of recovery. Patients often experience swelling, stiffness, and soreness around the knee. This pain is managed through a combination of medications, physical therapy, and cold therapy to reduce swelling. Over time, the intensity of pain generally decreases, although some individuals may experience lingering pain or stiffness for a longer period. Long-term outcomes usually include significant pain reduction and improved mobility, but in some cases, chronic pain can occur due to complications such as implant loosening, infection, or scar tissue. On the other hand, knee arthroscopy is a minimally invasive procedure used to diagnose and treat issues like meniscal tears or ligament damage. Post-arthroscopy pain is generally milder than after TKA due to the less invasive nature of the procedure. Patients may experience mild to moderate pain, swelling, stiffness, or discomfort when moving the knee. Pain management typically includes over-the-counter medications, rest, icing, and physical therapy to restore range of motion and strength. Recovery from knee arthroscopy is usually quicker, but some individuals may still experience lingering discomfort or complications like joint stiffness or infection. In both surgeries, while pain is expected in the initial recovery, prolonged or severe pain may signal complications and should be evaluated by a healthcare provider.
- Sprained & Torn Ligaments: A knee ligament sprain occurs when one of the ligaments that support the knee joint is stretched or partially torn due to excessive force, such as twisting or sudden impact. Ligaments are strong bands of tissue that connect bones and provide stability to the knee. A sprain typically happens during activities that involve sudden changes in direction, landing awkwardly, or direct blows to the knee. Sprains are categorized into three grades: Grade 1 involves mild stretching with no tear, Grade 2 is a partial tear, and Grade 3 is a complete tear of the ligament. Common symptoms of a sprain include pain, swelling, and difficulty moving the knee, although the knee may still remain somewhat functional depending on the severity of the injury. A torn knee ligament, on the other hand, involves a more severe injury where the ligament is completely or partially torn. This is most commonly seen with ligaments like the anterior cruciate ligament (ACL), medial collateral ligament (MCL), or posterior cruciate ligament (PCL). A torn ligament usually causes intense pain, swelling, instability (a feeling that the knee is giving way), and an inability to bear weight on the affected leg. These injuries often occur during sports activities or accidents that involve sharp pivoting, twisting motions, or direct trauma to the knee.
- Patellar Tendonitis: Prepatellar bursitis and patellar tendonitis are both conditions that affect the front of the knee, but they involve different structures and have distinct causes. Prepatellar bursitis is inflammation of the prepatellar bursa, a small fluid-filled sac located in front of the kneecap (patella). The bursa acts as a cushion between the skin and the kneecap, reducing friction when the knee moves. Prepatellar bursitis is often caused by prolonged pressure on the knee, frequent kneeling, or direct trauma to the area, earning it the nickname “housemaid’s knee” or “carpenter’s knee.” Symptoms include swelling, tenderness, and warmth over the kneecap, with fluid buildup causing the area to appear puffy. The condition may cause discomfort during knee movement, but the joint itself typically remains functional. In more severe cases, infection can occur, leading to redness and increased pain. Patellar tendonitis, also known as jumper’s knee, is inflammation or injury to the patellar tendon, which connects the kneecap (patella) to the shinbone (tibia). This condition is common in athletes who frequently jump or engage in repetitive stress activities like running or squatting. Patellar tendonitis causes pain just below the kneecap, which tends to worsen with activity and improve with rest. Over time, if left untreated, the tendon can weaken and possibly tear, leading to more serious complications. The pain is typically sharp and worsens with knee extension or heavy physical activities that involve the lower body. Effusion refers to the abnormal accumulation of fluid within the knee joint, often referred to as “water on the knee.” Effusion can occur as a result of many knee issues, including prepatellar bursitis, patellar tendonitis, ligament injuries, or arthritis. When there is effusion, the knee appears swollen, stiff, and can be painful, especially with movement. Effusion indicates inflammation or injury within the knee and can limit mobility.
- Patellofemoral Pain Syndrome: Patellofemoral pain syndrome (PFPS), often referred to as “runner’s knee,” is a condition characterized by pain around the front of the knee, particularly where the patella (kneecap) meets the lower end of the femur (thigh bone) at the patellofemoral joint. The pain is typically caused by irritation or inflammation of the soft tissues around the patella or due to the improper tracking of the patella during movement. This condition is common among athletes, especially runners, cyclists, and individuals who engage in activities that involve repetitive knee movements, such as squatting or stair climbing. However, it can also occur in non-athletes due to muscle imbalances, overuse, misalignment of the kneecap, or poor biomechanics. Symptoms of patellofemoral pain syndrome include a dull, aching pain in the front of the knee, especially when sitting for long periods (theater sign), climbing stairs, squatting, or kneeling. The pain may worsen with activity and is often accompanied by a grinding or clicking sensation in the knee.
- Meniscus Tear: A meniscus tear is an injury to one of the two crescent-shaped pieces of cartilage located in the knee joint, known as the menisci. These menisci act as shock absorbers between the thigh bone (femur) and shinbone (tibia) and help distribute body weight across the knee joint, providing stability and cushioning during movement. Meniscus tears commonly occur due to a sudden twisting or pivoting motion, often during sports activities like football, basketball, or soccer, though they can also result from degenerative wear and tear over time, particularly in older adults. There are different types of meniscus tears, including longitudinal, bucket-handle, radial, and flap tears, each depending on the location and severity of the damage. Symptoms of a meniscus tear include pain, swelling, and stiffness in the knee. Many people with a torn meniscus may experience a “popping” sensation at the time of the injury, followed by difficulty moving or straightening the knee. The knee may feel like it’s locking, catching, or giving way, especially during activity.
- Iliotibial Band Syndrome: Iliotibial Band Syndrome (ITBS) is an overuse injury that causes pain along the outer side of the knee, and it commonly affects runners, cyclists, and other athletes who engage in repetitive leg movements. The iliotibial (IT) band is a thick band of connective tissue that runs from the hip, along the outer thigh, and down to the shin, helping stabilize the knee joint during movement. In ITBS, the IT band becomes irritated and inflamed due to friction as it repeatedly rubs against the outer part of the knee (the lateral femoral condyle) during activities like running or cycling. This irritation is often the result of biomechanical issues such as improper running form, muscle imbalances, tightness in the hip or thigh muscles, or overtraining. Symptoms of ITBS typically include sharp or burning pain on the outside of the knee, which tends to worsen during physical activities that involve bending the knee, such as running downhill or climbing stairs. The pain may start mildly but can become more severe and persistent if not addressed.
- Chondromalacia: Chondromalacia refers to the softening and breakdown of the cartilage on the underside of the kneecap (patella), leading to pain and discomfort in the front of the knee. The condition is also commonly known as chondromalacia patellae or “runner’s knee.” The cartilage, which normally helps the knee joint move smoothly, becomes damaged, causing friction between the kneecap and the femur (thigh bone) during movement. Chondromalacia is often caused by overuse, improper alignment of the kneecap, muscle imbalances, or injury to the knee. It’s common among young athletes, particularly runners, cyclists, and those involved in activities that involve a lot of knee bending, but it can also affect older adults due to wear and tear over time. Symptoms include a dull, aching pain in the front of the knee, especially during activities like climbing stairs, squatting, kneeling, or after sitting for long periods with bent knees. Some people may also feel a grinding or clicking sensation in the knee when bending it.
Frequently Asked Questions
Have more questions? Schedule a consultation with Dr. Patel to gain additional insights and discuss treatment options. We are committed to advancing your health through patient education and a safe, minimally invasive approach.
Knee pain is diagnosed through a combination of a patient’s medical history, physical examination, and diagnostic tests. During the exam, a doctor will assess the knee’s range of motion, stability, and tenderness, while checking for swelling, warmth, or deformities. The patient’s symptoms, activities, and any prior injuries are also discussed to identify potential causes. Diagnostic imaging, such as X-rays, MRIs, or CT scans, may be used to visualize bone, cartilage, and soft tissue damage, while ultrasound can help detect issues like bursitis or tendonitis. In some cases, blood tests or joint fluid analysis may be performed to rule out infections or conditions like gout or arthritis.
Treatment options for knee pain depend on the underlying cause and severity. Conservative treatments include rest, ice, compression, and elevation (RICE) to reduce swelling and pain. Over-the-counter pain relievers, such as NSAIDs, can help manage inflammation. Physical therapy is often recommended to strengthen the muscles around the knee and improve mobility. For more severe cases, corticosteroid injections or hyaluronic acid injections may be used to relieve pain and inflammation. In cases of structural damage, such as ligament tears or advanced arthritis, surgical options like arthroscopy or total knee replacement may be necessary. Lifestyle modifications, such as weight management and activity adjustments, can also help manage knee pain.
The duration of knee pain varies depending on the cause and severity of the injury or condition. Acute knee pain from minor injuries, such as a sprain or strain, may last a few days to a few weeks with proper treatment. Chronic conditions, like arthritis or tendinitis, can cause ongoing pain that lasts for months or years, with flare-ups that vary in intensity. Post-surgical knee pain, such as after knee replacement or arthroscopy, typically improves over several weeks to months as the knee heals. The length of recovery and pain relief depends on factors like the treatment approach, individual healing, and adherence to rehabilitation.
Untreated or poorly managed knee pain can lead to complications. These may include chronic pain, reduced mobility, muscle weakness, and joint instability, which can limit daily activities and physical function. Over time, persistent knee pain can also contribute to compensatory movement patterns, potentially leading to issues in other joints, such as the hips or lower back. In severe cases, untreated conditions like ligament tears or advanced osteoarthritis may cause permanent joint damage, increasing the likelihood of needing surgery, such as knee replacement. Early diagnosis and proper management are essential to prevent these complications.
Gramercy Center
Take the first step towards a healthier life by scheduling your initial consultation with Dr. Patel. At our clinic, we specialize in minimally invasive procedures that offer faster recovery, improved function, and decreased pain. Our client-centered approach ensures that you receive the highest quality care tailored to your unique needs. We look forward to offering you an exceptional experience.